Knee Microfracture Surgery
Autologous Chondrocyte Implantation (ACI) is a surgical technique employed to address full-thickness cartilage defects in the knee. This minimally invasive procedure harnesses the body's innate regenerative capabilities to promote the healing and restoration of the damaged chondral surface.
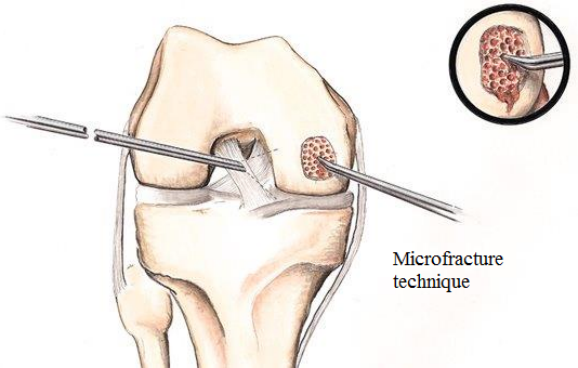
What Are the Symptoms of An Articular Cartilage Injury That Can Be Treated with Microfracture Surgery?
- Persistent intermittent swelling in the knee.
- Discomfort or pain when engaging in extended walking or climbing stairs.
- Occasional instability or giving way of the knee under weight-bearing.
- The presence of loose cartilage fragments that may impede knee joint movement, resulting in locking or restricted range of motion.
- Audible joint noises , often described as "snap, crackle, or pop," particularly if the cartilage behind the kneecap is affected, leading to crepitus during motion.
After Articular Cartilage Damaged Has Been Diagnosed, What Factors Indicate Microfracture?
- A patient presents with a complete-thickness defect located either in a weightbearing region situated between the femur and tibia or in a region of contact between the rear of the patella.
- The patient exhibits compromised cartilage integrity, unable to adequately protect the underlying bone.
- The patient displays degenerative knee alterations, despite having a typically aligned knee structure.
What factors Should be Considered Before Microfracture Surgery?
In general, microfracture procedures yield optimal results when applied to cartilage defects surrounded by healthy cartilage, a condition referred to as good "containment." Furthermore, microfractures tend to excel in treating smaller cartilage defects, typically measuring less than 2 cm2 in size. Larger cartilage defects may necessitate the use of a fresh Osteoarticular Allografts to offer the patient the best chance of a favorable outcome.
How is Microfracture Surgery Performed?
Microfracture surgery is a minimally invasive procedure commonly performed through arthroscopy. This technique is particularly effective when addressing issues at the end of the femur (thigh bone), where outcomes are generally more predictable. However, the size of the defect being treated plays a crucial role, as smaller defects tend to yield more durable fibrocartilage scar tissue in the microfracture area.
The essence of microfracture surgery lies in creating tiny holes, typically spaced about 3 to 4mm apart, in the exposed bone. These holes serve the purpose of releasing stem cells, which subsequently form a clot within the microfracture site. This clot, enriched with marrow, becomes the foundation for new tissue growth. The microfracture technique intentionally produces a roughened bone surface that promotes better adherence of the clot. Over time, this clot matures into a firm, smooth, and durable repair tissue.
In the initial phase, the clot is vulnerable to displacement if the patient puts too much weight on the treated area or engages in strenuous activities. Consequently, patients are usually advised to remain non-weightbearing for approximately six weeks following microfracture surgery. Additionally, maintaining continuous motion over the microfracture site can help the new tissue conform better to the contours of the bone's end. To facilitate this, continuous passive motion machines (CPM) are often used postoperatively to ensure optimal contouring and healing of the microfractured area.
What is Microfracture Recovery Like?
Rehabilitation following microfracture surgery is a critical component for optimizing the outcome of this procedure. Typically, weightbearing is gradually reintroduced around the six-week mark post-surgery. During this period, it is imperative to follow a carefully paced progression of weightbearing to allow the microfracture tissue to undergo the necessary hardening process. Rushing into activities too soon after microfracture recovery can have detrimental effects, potentially hindering the healing process or resulting in the formation of soft fibrocartilage.
Should the microfracture heal in a softer state, despite covering the bone's end, it may not function effectively, and patients may experience recurring pain. The specific timeline for recovery can vary based on the location of the microfracture and the size of the initial defect. Generally, patients can expect a healing period spanning from four to seven months before they can safely increase their activities and potentially engage in occasional impact activities.
In essence, the rehabilitation program plays a pivotal role in the success of microfracture surgery, ensuring that the newly formed tissue has the time and conditions necessary to develop into a robust and functional state, ultimately offering patients the best chances for a successful recovery.
Is microfracture a “cure” for osteoarthritis?
Indeed, microfracture is a specialized technique designed to address chondral defects by promoting the formation of a new surface. When this procedure proves successful, it often results in reduced pain and swelling, ultimately leading to improved joint function.
In a similar vein, microfracture can be likened to a transformative process aimed at rejuvenating damaged joint surfaces. Its success hinges on its ability to create a renewed and functional area, offering patients relief from discomfort and enhancing their overall joint mobility.
Is the new tissue that forms after the microfracture identical to the original articular cartilage?
Certainly, the newly formed tissue resulting from microfracture surgery can be described as a unique blend, combining characteristics of articular-like cartilage and fibrocartilage. Over time, clinical experience has demonstrated that this hybrid tissue exhibits remarkable durability and often functions comparably to native articular cartilage.
This distinctive tissue composition underscores the effectiveness of microfracture as a surgical technique, as it yields a robust and functional replacement surface that can significantly enhance joint performance and alleviate discomfort for patients.
